Introduction
Diabetes is no longer a rare condition, it is a fast-growing lifestyle disease affecting millions worldwide. Whether you are trying to prevent it, manage early symptoms, or understand your risk, knowing the symptoms and causes of diabetes is the first step toward better health.
In this guide, Diabetes Symptoms & Causes you will learn how to identify early warning signs, what causes diabetes, and how your daily habits may be silently influencing your blood sugar levels.
What Is Diabetes?
Diabetes Mellitus is a condition where your body either does not produce enough insulin or cannot effectively use it. Insulin is a hormone that regulates blood sugar (glucose), which your body uses for energy.
When insulin does not work properly, glucose builds up in the bloodstream—leading to serious health complications over time.
Common Symptoms of Diabetes
Recognising symptoms early can prevent long-term damage. Unfortunately, many people ignore these warning signs until the condition worsens.
1. Frequent Urination (Polyuria)
One of the earliest signs is increased urination, especially at night. Excess sugar in your blood forces your kidneys to work harder, leading to increased urine production.
What is Frequent Urination?
Frequent urination, medically referred to as polyuria, is commonly experienced by individuals managing diabetes. This condition is characterized by the production of excessive volumes of urine, which can lead to numerous health complications if not addressed properly.
The Link Between Diabetes and Polyuria
In diabetic patients, elevated blood glucose levels often exceed the renal threshold, prompting the kidneys to filter out excess glucose alongside water. This results in increased urine output, which is why polyuria is frequently observed in diabetes care. Understanding this relationship is essential for effective management of the condition and for mitigating any potential health risks.
Managing Frequent Urination
Addressing polyuria involves strict monitoring of blood glucose levels and ensuring they remain within the target range. Patients are encouraged to maintain a balanced diet and engage in regular physical activity to help regulate blood sugar. Additionally, staying hydrated can assist in managing this condition, although excessive fluid intake should be avoided to minimize bathroom trips. Regular check-ups with healthcare professionals are vital in developing an individualized management plan tailored to each patient’s needs.
In conclusion, managing frequent urination is a crucial aspect of diabetes care. Increased awareness and proactive measures can significantly improve a patient’s quality of life and prevent further complications related to this diabetes symptom.
2. Excessive Thirst (Polydipsia)
As your body loses more fluids, you feel constantly thirsty, even after drinking water. Excessive Thirst creates a cycle of dehydration.
What is Polydipsia?
Polydipsia, commonly known as excessive thirst, is a condition that compels individuals to drink more fluids than usual. This increased thirst can be a symptom of various underlying health issues, making it crucial to understand its causes and implications.
Causes of Excessive Thirst
There are several reasons why someone might experience polydipsia. It can stem from simple causes such as dehydration, which might occur due to hot weather or vigorous exercise. However, polydipsia can also be a sign of more serious conditions like diabetes mellitus or kidney disorders. In fact, individuals with uncontrolled diabetes may experience high blood sugar levels that trigger a desperate need for water.
When to Seek Help
If you find yourself constantly thirsty regardless of how much water you consume, it’s essential to consult with a healthcare professional. Persistent excessive thirst can indicate a significant health issue that requires diagnosis and management. Early detection and treatment can help prevent more severe health complications associated with underlying conditions linked to polydipsia.
3. Increased Hunger (Polyphagia)
Despite eating regularly, your body may not be able to use glucose efficiently, leaving you feeling hungry all the time.
What is Polyphagia?
Polyphagia, commonly known as increased hunger, is a prevalent symptom among individuals with diabetes. This condition arises when the body fails to efficiently utilize glucose for energy, leading to persistent feelings of hunger, even after eating adequate amounts of food. Understanding the underlying mechanisms of polyphagia is critical for effective diabetes management.
Causes of Increased Hunger in Diabetes
In people with diabetes, polyphagia is often linked to high blood sugar levels. When insulin is insufficient or ineffective, glucose remains in the bloodstream instead of entering the cells, causing the body to signal hunger as it craves energy. Additionally, the process of ketosis, where the body starts to break down fat for energy due to a lack of insulin, can also contribute to feelings of hunger. These processes can lead to a vicious cycle of overeating and further complications in blood sugar management.
Managing Polyphagia in Diabetes Care
Effectively addressing polyphagia involves a combination of lifestyle adjustments and proper medical care. Individuals with diabetes should focus on consuming balanced meals rich in fibers and proteins, as these can help maintain satiety for longer periods. Regular monitoring of blood glucose levels and adherence to prescribed medication regimens are equally crucial. For anyone experiencing persistent increased hunger, consulting with a healthcare professional can provide personalized strategies for better managing their condition.
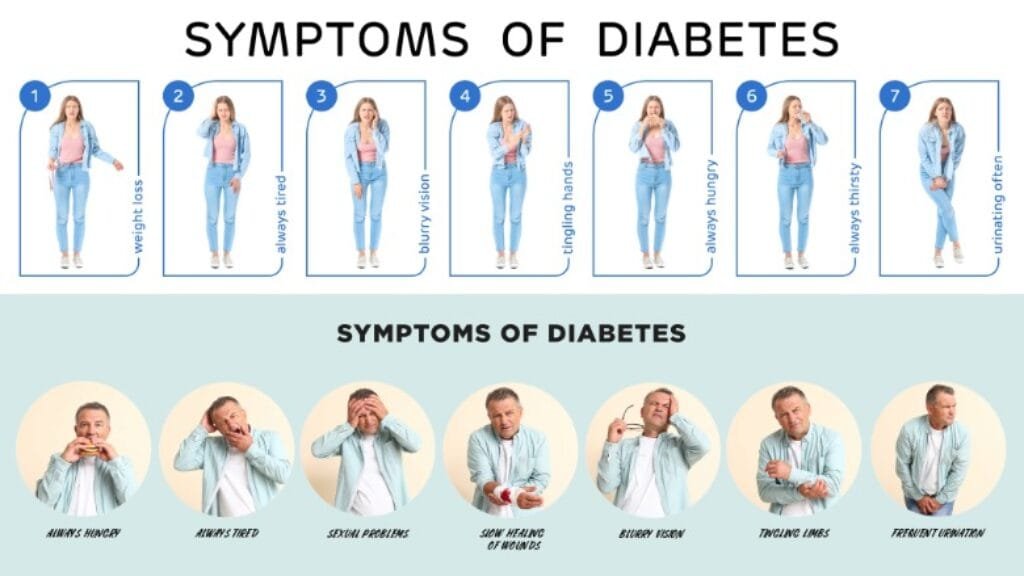
4. Unexplained Weight Loss
Sudden weight loss, especially in Type 1 Diabetes, can occur because your body starts breaking down fat and muscle for energy.
5. Fatigue and Weakness
Without proper glucose absorption, your body lacks energy. This leads to constant tiredness, even after adequate rest.
6. Blurred Vision
High blood sugar levels can affect the lenses of your eyes, leading to temporary vision problems.
7. Slow Healing Wounds
Cuts, infections, or bruises that take longer to heal may indicate poor blood circulation and high glucose levels.
8. Frequent Infections
Cuts, infections, or bruises that take longer to heal may indicate poor blood circulation and high glucose levels.
8. Tingling or Numbness in Hands & Feet
This symptom is associated with nerve damage, which commonly occurs in individuals who have had Type 2 Diabetes for an extended period.
Early Warning Signs You Should NOT Ignore
Many individuals have prediabetes without knowing it. Look out for:
- Dark patches on skin (especially neck or armpits)
- Mild but persistent fatigue
- Slight increase in thirst or urination
- Gradual weight gain around the abdomen
These subtle signs can progress into full diabetes if ignored.
Main Causes of Diabetes
Understanding the root causes helps you prevent or delay the condition.
1. Insulin Resistance
The most common cause of Type 2 Diabetes is insulin resistance. Your body produces insulin, but your cells do not respond properly.
What triggers it?
- High sugar and processed food intake
- Sedentary lifestyle
- Obesity, especially belly fat
2. Genetic Factors
If diabetes runs in your family, your risk increases significantly. However, genetics alone do not guarantee the condition, lifestyle plays a key role.
3. Autoimmune Response
In Type 1 Diabetes, the immune system mistakenly attacks insulin-producing cells in the pancreas. This is not preventable and usually develops early in life.
4. Poor Diet and Lifestyle
Your daily habits are one of the biggest contributors
- Excess sugar and refined carbs
- Lack of physical activity
- Irregular sleep patterns
- Chronic stress
5. Obesity and Belly Fat
Fat accumulation, especially around the abdomen, interferes with insulin function. This is one of the strongest risk factors for developing diabetes.
6. Hormonal Imbalances
Conditions like Polycystic Ovary Syndrome increase insulin resistance, raising diabetes risk, especially in women.
7. Age Factor
As you age, your metabolism slows down, and your body becomes less efficient at using insulin. People over forty are at higher risk.
8. Stress and Sleep Disorders
Chronic stress increases cortisol levels, which can raise blood sugar. Poor sleep also disrupts metabolic health.
Types of Diabetes You Should Know
1. Type 1 Diabetes
- Autoimmune condition
- Requires insulin therapy.
- Usually diagnosed in children or young adults.
2. Type 2 Diabetes
- Most common type
- Linked to lifestyle and insulin resistance.
- Early intervention can frequently control or even reverse the condition.
3. Gestational Diabetes
- Occurs during pregnancy.
- Usually temporary, but it increases future risk.
Who Is at High Risk?
You may be at higher risk if you:
Are overweight or obese.
Have a family history of diabetes.
Live a sedentary lifestyle.
Have high blood pressure or cholesterol.
Have conditions like PCOS.
When Should You See a Doctor?
- Persistent fatigue or thirst
- Sudden weight changes
- Frequent infections
- Vision issues






