If you’ve ever dealt with gut issues that just don’t seem to go away, you know how frustrating it can be. One day you feel fine… the next, your stomach turns against you. That’s the reality for people living with inflammatory bowel disease (IBD).
And here’s the confusing part: most “healthy eating advice” doesn’t always apply here. You’re told to eat more fruits, vegetables, and fibre… but sometimes those very foods can make things worse.
So what actually works? Let’s break it down in simple terms.
What Is Inflammatory Bowel Disease (IBD)?
IBD isn’t just a sensitive stomach. It’s a long-term condition in which the digestive tract remains inflamed. This inflammation doesn’t come and go quickly; it can last for weeks, months, or even years.
- Persistent abdominal pain
- Frequent diarrhoea
- Loss of appetite
- Constant fatigue
Some people even experience phases when symptoms disappear completely… only to return later.
Crohn’s disease
Ulcerative colitis
Both affect the gut—but in different ways.
Crohn’s Disease vs Ulcerative Colitis: What’s the Difference?
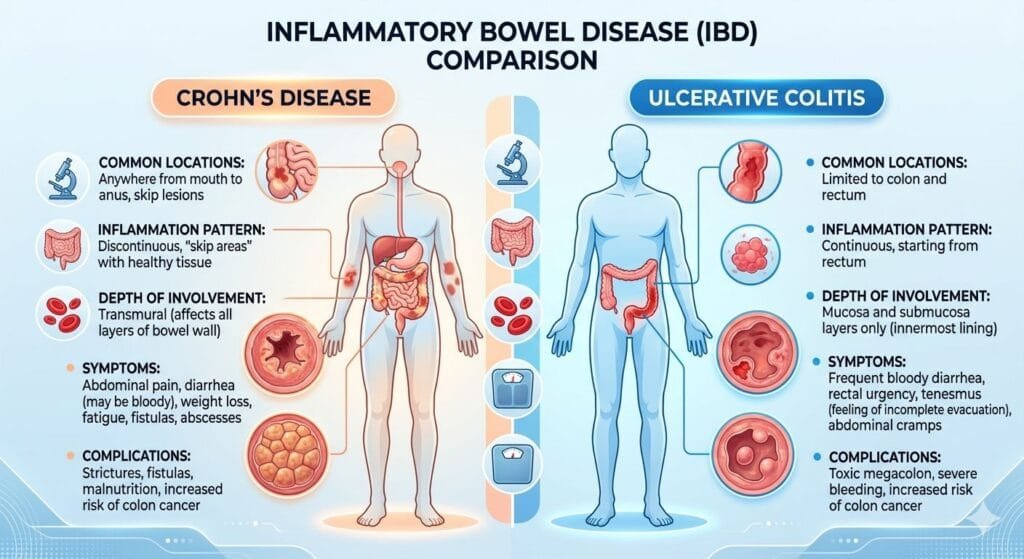
Understanding this matters because diet responses can differ.
Crohn’s Disease
- Affects all layers of the intestinal wall
- Usually impacts the small intestine
- Reduces nutrient absorption
- Often leads to chronic diarrhoea
In simple terms, your body struggles to absorb what you eat.
Ulcerative Colitis
- Affects only the inner lining of the large intestine (colon)
- Disrupts water absorption
- Causes diarrhoea and discomfort
Think of it as the colon losing its ability to “finish the job” properly.
Why Does Diet Feel So Confusing with IBD?
Here’s where most people get stuck.
You’re told:
- Eat clean
- Eat fiber
- Eat fresh
But with IBD, those “healthy” foods can sometimes trigger flare-ups. That’s because your gut is already inflamed and sensitive. Even small irritants can cause a reaction. So instead of following generic diet rules, the goal shifts to something more practical:
👉 Inflammatory Bowel Disease Diet – Eat what your gut can tolerate, not what looks healthy on paper
The Real Goal: Calm the Gut, Not Just Feed It
Food won’t cure IBD. That’s important to understand upfront. But the right diet can make a noticeable difference in how you feel day to day.
A smarter approach focuses on:
- Reducing inflammation
- Supporting gut bacteria
- Avoiding trigger foods
- Preventing nutrient deficiencies
This is less about “perfect eating” and more about strategic eating.
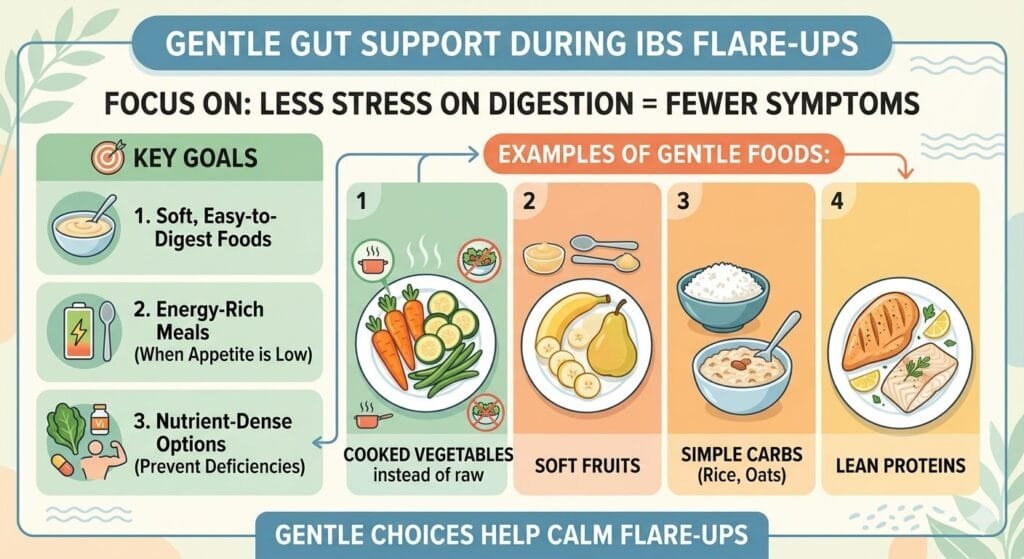
Best Foods for IBD (When Your Gut Is Sensitive)
During flare-ups, your gut needs gentle support.
Focus on:
- Soft, easy-to-digest foods
- Energy-rich meals (since appetite may be low)
- Nutrient-dense options to prevent deficiencies
Examples:
- Cooked vegetables instead of raw ones
- Soft fruits (like bananas)
- Rice, oats, and simple carbs
- Lean proteins
The idea is simple:
👉 Less stress on digestion = fewer symptoms
Foods That Commonly Trigger Flare-Ups
This varies from person to person, but some common triggers include:
- Spicy foods
- Raw vegetables
- High-fibre foods (during flare-ups)
- Dairy (for some people)
- Processed or greasy foods
Interestingly, your original content highlights that even healthy foods like fresh fruits and vegetables may need to be limited at times. That’s not forever, but during sensitive phases, it can help.
Why a Food Diary Is More Powerful Than Any Diet Plan
Here’s a simple truth most people ignore: 👉 No one diet works for everyone with IBD. What helps one person might trigger symptoms in another. That’s why keeping a food diary is one of the smartest things you can do.
Track:
- What you eat
- When you eat
- How do you feel afterwards
Over time, patterns start to show. And once you know your triggers, everything becomes easier
What About Surgery and Long-Term Gut Sensitivity?
In more severe cases, surgery may be required.
As mentioned in your document, many people eventually undergo procedures to remove damaged parts of the intestine. After that, the gut can become even more sensitive. Which makes diet even more important—not stricter, but smarter.
Do You Need Supplements?
Because of poor nutrient absorption, deficiencies are common in IBD. You may need:
- Vitamins
- Minerals
- Specific supplements
But this isn’t something to guess. 👉 Always work with a doctor before adding supplements.
The Bottom Line: Keep It Practical, Not Perfect
Living with IBD isn’t about following a perfect diet. It’s about understanding your body. Some days your gut will tolerate more. Some days it won’t. That’s normal. Instead of chasing “ideal eating,” focus on:
- What reduces your symptoms
- What keeps your energy up
- What your body actually accepts
Because at the end of the day…
👉 The best diet for IBD is the one your gut agrees with.







